Fascia
Fascia. Many of you have likely heard this term used more and more over recent years. This is perhaps due to the surge of new research on the topic and therefore the renewed interest within the manual medicine community.
What is Fascia?
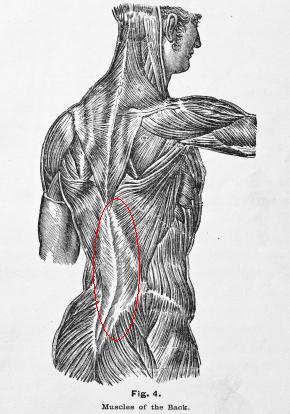
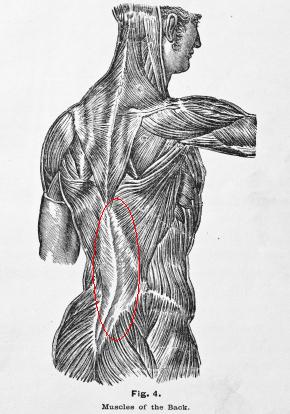
Fascia can be defined as a sheet or band of fibrous connective tissue enveloping muscles, organs and other soft tissue structures of the body. Fascia is divided into three separate layers that work closely with one another. The most superficial layer (fascia superficialis) lies directly beneath the skin. The middle layer (fascia profundus) has connections with fascia superficialis and directly overlies the muscles. The deepest layer (deepest fascia or dural tube) directly surrounds and protects the central nervous system.
Why do we care about fascia?
The medical community has long known about the existence of fascia, however, the role that it plays in movement and biomechanics of soft tissues has often been overlooked. In order to understand this important role, you must first understand the complex anatomy of the layers themselves and their relationship with the other. For the purpose of this blog we’ll keep it short and simple, focusing on the 2 most superficial layers.
Dysfunction in Fascia
Although the primary function of fascia is to sustain and protect the underlying soft tissue with strong connections, it is imperative that each layer maintain a certain degree of independent motion. This is necessary so that our skin has the ability to slide along the muscle as well as all the muscle fibres among themselves. If this were not the case, we would not be able to move our joints to the extent that we can as they would be limited by our skin and muscles.
The Effect of Scar Tissue
So why has there been a shift in focus to fascia when it comes to soft tissue injuries? When a soft tissue injury occurs a process takes place to heal the area which involves alterations to the connective tissue. This process includes the formation of tissue fibrosis and scarring (scar tissue). This scarring within the connective tissue or fascia creates not only a relative weakness in the area (as the new connective tissue has less tensile strength and non uniform alignment) but also creates a bond between tissue layers, leaving a lack of relative movement in the area.
Graston Technique
The focus of treatment for these injuries is to break up the scar tissue at the site of the injury and encourage a proper reorganization of the surrounding connective tissue and fascia. Methods that we commonly use to treat soft tissue injuries involving the fascia are Graston Technique, Active Release Technique and Low Intensity Laser Therapy. If you have a soft tissue injury that just doesn’t seem to be getting better, or an injury that seems to get better but somehow returns, it could mean that there is a change in the fascia or connective tissue in the area which must be returned to normal before proper function can be restored!
Our Burlington Clinic can be reached at – info@burlingtonsportstherapy.com
References
Van der Wal, J. The Architecture of the Connective Tissue in the Musculoskeletal System – An Often Overlooked Functional Parameter as to Proprioception in the Locomotor Apparatus. International Journal of Therapeutic Massage and Bodywork 2009; 2(4):1-15.
Spina, Andreo. Targeting Fascia – Rethinking the approach of soft-tissue treatment. Canadian Chiropractor 2011; 16(3):27-29