Calcific Tendinopathy
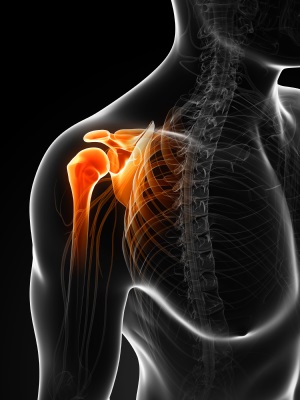
Calcific tendinopathy is a condition that involves calcific deposition in our soft tissues. Most often it affects the shoulder, and specifically, it likes to target the rotator cuff tendons. Approximately two-thirds of cases affect a rotator cuff muscle called the supraspinatus. There are still quite a few aspects of calcific tendinopathy that are unknown. For example, for some people, the calcification seems to disappear over time. For others, this does not happen. We don’t know why this co-operates for some people while for others it does not. At the same time, some people have calcifications within their tendons and have no pain while others experience significant pain as a result of calcific tendinopathy. Sometimes there is also a tear in a shoulder tendon, as rotator cuff tears occur along with the calcification in the tendon for approximately 25% of patients.
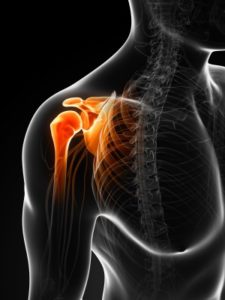
Calcific Tendinopathy
As mentioned above, we don’t really know for certain why calcific tendinopathy happens. We do know that it occurs more frequently in diabetics and those with thyroid disorders. Otherwise, we only have theories as to why it occurs. One leading theory is that placing repetitive demands on the tendon leads to a cellular environment that promotes the calcific deposits, a theory that is based on histopathologic studies. Regardless of the actual cellular mechanism, what seems to have been established is that inflammatory cells are absent with calcific tendinopathy. This means that strategies focusing on reducing inflammation (modalities, ice, and anti-inflammatories) are unlikely to improve the situation.
Calcific tendinopathy can be diagnosed through x-ray or ultrasound. For most people, it would be fair to expect a course of treatment having already been done as the practitioner would expect it to behave like a minor rotator cuff tendinopathy without the suspicion of a significant tear. Perhaps many get referred for imaging once a course of conservative care fails which then makes it more apparent that the patient has calcific tendinopathy.
Treatment Options for Calcific Tendinopathy
There are various treatment options for calcific tendinopathy. Most people don’t require surgery and can be treated conservatively (by a physiotherapist, chiropractor or athletic therapist, for example). In fact, 90% of patients seem to respond well to conservative treatment and don’t need surgery. For some patients, medications and cortisone injections are appropriate for their condition. Cortisone can often help with reducing the pain associated with calcific tendinopathy. However, according to the literature, it does not help in eliminating the calcium in the tendon.
From my clinical experience, I have found that this condition often coincides with adhesive capsulitis or “frozen shoulder”. If you have significant pain and significant loss of motion in a shoulder with no major tearing but lots of calcium in the tendons, this really raises the suspicion of frozen shoulder. Surgery for calcific tendinopathy is rare. It can range from arthroscopic surgery or needle lavage to open surgery. There seems to be some debate in the research as to whether removal of all the calcium is even necessary. Regardless, surgery is only required for approximately 10% of cases, but it does seem to show some benefit.
In summary, calcific tendinopathy is a relatively common condition that might be the cause of some cases of shoulder pain. It doesn’t necessarily have to affect the shoulder. It is diagnosed through the combination of imaging and clinical suspicion, often after a course of conservative treatment has not changed the pain significantly. It can often be associated with frozen shoulder, and it is more common in diabetics and those with thyroid conditions. It can be treated successfully without surgery (through physiotherapy, chiropractic and athletic therapy as an example) and usually the condition leaves the shoulder the same way it was at the very beginning…there may not be any long-term consequences of the condition.
By: Dr. Kevin McIntyre B.Kin., DC
Oliva F, Via AG, Maffulli N. Calcific tendinopathy of the rotator cuff tendons. Sports Medicine & Arthroscopy Reviews 2011; 19(3): 237-243.