Facet Joints in Neck and Back Pain
There are many different causes for back and neck pain. Quite often, patients discuss the different layers of causation. For example, “my hip flexors are tight so my back hurts” or “my pelvis is shifted which is causing me pain”. Although these situations may or may not be happening, they are not necessarily an actual diagnosis. More often than not, the diagnosis of neck and back pain identifies the primary pain generator. For neck pain and back pain, one of the most common pain generators (and therefore one of the most common diagnoses) involves the facet joint.
The Facet Joint – What is it?
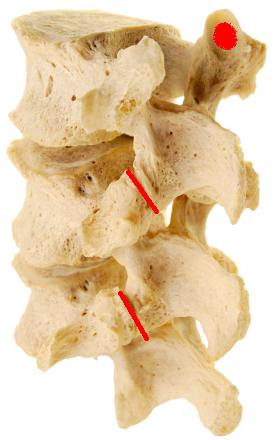
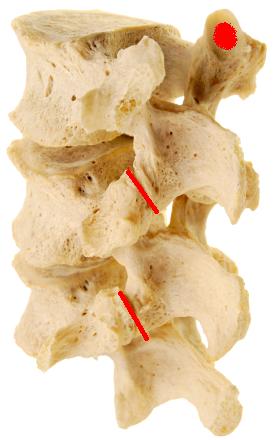
In the picture, the facet joint is highlighted in red. It is rather predictable that the facet joint is such a common pain generator for neck and back pain; we have two facets at almost every level of the spine, and these joints play an integral role with almost every movement we make. They also have ample innervation. This means that the many nerve endings in the joint are able to sense dysfunction and generate a significant amount of pain.
Facet Joint Symptoms
The symptoms of facet joint syndrome can be variable. In general, the person with facet joint pain has an achy, throbbing pain in the neck or lower back that can also feel sharp with certain movements. Rotation and extension (especially combined) are usually the most painful movements, but as mentioned above, the facet joint is involved with almost every spinal movement. Therefore, an irritated facet joint will usually generate some level of pain with any movement. If a facet joint becomes significantly irritated, the patient can experience symptoms in the arm or legs. This can be referred pain or can even irritate the adjacent nerve structures and generate symptoms of numbness, tingling, pins and needles.
Diagnosis of Facet Joint Pain
X-rays are usually not helpful in the diagnosis of common facet joint pain. That being said, arthritic degeneration of the facet joints can be seen on x-ray which can be helpful for the doctor in determining its role in a patient’s condition. A common orthopedic test that the doctor will use in the clinic is the Kemp’s or Quadrant test. This test compresses the facet joint and gives the practitioner an idea as to whether or not the facet joint is involved. To perform this test, the person rotates and extends the spine on the side of irritation to see if the pain is increased. It is important to remember that this test is not guaranteed to be accurate all the time. A knowledgeable practitioner will combine it with the other information gathered in the examination to arrive at the diagnosis of facet joint dysfunction.
Facet Joint Treatment
It is reasonable to suggest that one of the best treatments for facet joint pain is the chiropractic adjustment. When a chiropractor adjusts the spine, they are usually targeting the facet joint. There is a large body of published research that supports the safety and effectiveness of spinal adjustments for the treatment of various spinal conditions, including facet joint dysfunction. An alternative to spinal adjustments are mobilizations of facet joints. This is a gentle procedure in which the practitioner moves the joint that is irritated to restore normal motion. As mentioned at the beginning of this blog, there are often accompanying changes in the spine that need to be addressed for complete resolution of facet joint syndrome. An example is muscular spasm. Quite often, the surrounding muscles tighten and “spasm” so soft tissue therapy is helpful to alleviate some of the symptoms. Modalities like laser can also be helpful in reducing the irritation or inflammation in the joint. Therefore, there are a wide variety of treatment options for facet joint pain. The most appropriate treatment for a given patient depends on a number of factors including (but not limited to) severity of the condition, duration of symptoms, location of pain, patient comfort with treatment and other pertinent health history.
Questions? Comments? Please don’t hesitate to contact us!
References
Gouveia L et al. Safety of chiropractic interventions: a systematic review. Spine 2009; 34(11): E405-13.
Schafer A et al. Classification of low back related leg pain – a proposed patho-mechanism based approach. Manual Therapy 2009; 14:222-230.