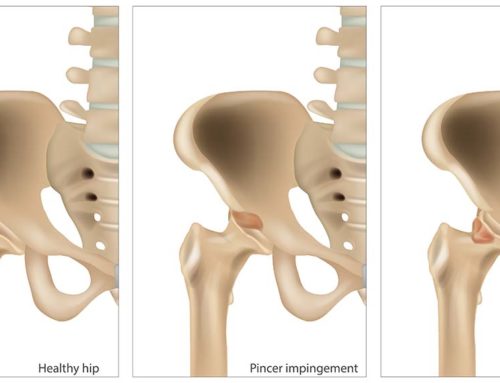
Frozen Shoulder
Shoulder pain is very common, affecting up to 26% of the population. There are many different causes of pain in the shoulder, one being frozen shoulder. Frozen shoulder has nothing to do with temperature. Frozen shoulder is a slang term that describes a condition in which the shoulder becomes very stiff and very painful. The technical term is adhesive capsulitis.
Frozen Shoulder Causes
Frozen shoulder is more common in females, especially between 40 and 65 years of age. Occasionally, it can be linked to other conditions like diabetes or thyroid conditions. Quite often, though, it starts for reasons unexplained in otherwise healthy individuals.
Frozen shoulder is painful. The hallmark of the condition, though, is reduced mobility. Keep in mind that this can happen with many shoulder conditions, but frozen shoulder is a little different. Astute clinicians can determine the subtle nuances associated with loss of movement in frozen shoulder. What makes the movement loss unique is that it primarily limits external rotation (twisting outward) and abduction (lifting up to the side). The movement loss with frozen shoulder should be more noticeable when the arm is moved by another person (passive movement). Imaging (like x-ray or MRI) is usually not helpful in diagnosing frozen shoulder but it can help to rule out other diagnostic possibilities.
There’s still a lot of mystery surrounding frozen shoulder. Some research suggests that the primary problem is inflammation, and some focuses on the new blood vessels in the area of the shoulder joint, while other research focuses on new nerve growth that occurs. Regardless, we do know that there are fibrotic changes in the joint area, which limit movement and cause plenty of pain!
Frozen shoulder is typically a gradual condition. Loss of motion occurs over a significant period of time. For some, stiffness can persist beyond a year (close to two years). For this reason, it can really impact a person’s lifestyle!
There are many different treatment options for frozen shoulder. Corticosteroid injections, interferential current, laser therapy, ultrasound, acupuncture, joint mobilization, manipulation, rehabilitative exercise, active release technique, graston technique…the list goes on. The generally accepted idea with treatment is to reduce pain and improve mobility. For many patients, this requires a reasonable amount of discomfort in moving the shoulder; however, in the long term, this facilitates a faster return to normal function.
References:
Kelley MJ, Shaffer MA, Kuhn JE et al. Shoulder pain and mobility deficits: adhesive capsulitis – clinical practice guidelines. Journal of Orthopedic & Sports Physical Therapy 2013; 43(5): A1-A31.
Chard MD, Hazleman R, Hazleman BL, King RH, Reiss BB. Shoulder disorders in the elderly: a community survey. Arthritis Rheum 1991; 34: 766-769.
Aydeniz A, Gursoy S, Guney E. Which musculoskeletal complications are most frequently seen in type 2 diabetes mellitus? J Int Med Res 2008; 36: 505-511.
Bridgman JF. Periarthritis of the shoulder and diabetes mellitus. Ann Rheum Dis 1972; 31: 69-71.
Balci N, Balci MK, Tüzüner S. Shoulder adhesive capsulitis and shoulder range of motion in type II diabetes mellitus: association with diabetic complications. J Diabetes Complications 1999; 13: 135-140.