Iliotibial Band Pain | Pain on the Outside of the Knee
By: Dr. Kevin McIntyre B.Kin., DC
If you have pain on the outside of your knee, you may be experiencing iliotibial band pain. The iliotibial band (ITB) is that thick, band-like structure you can feel on the side of your thigh. It is not a muscle, but two muscles contribute to forming the ITB. The tensor fascia latae (TFL) and the gluteus maximus both blend their fibres from the pelvis into the ITB, which then travels down the side of the thigh to just below the knee. The function of the ITB is not entirely certain, but studies suggest that while walking, it helps stabilize the hip and knee and stores some elastic energy.
Cause and Diagnosis of ITB Pain
Acute injuries to the ITB are very rare. Most injuries take a while to develop, often from activities like running. In fact, ITB pain accounts for up to 14% of all running-related injuries. Imaging isn’t necessary to diagnose ITB dysfunction, and, unfortunately, clinical orthopedic tests aren’t very reliable. Most cases are diagnosed through a thorough discussion and some palpation of the area to decipher the exact pain location. The most common finding is pain on the outside of the knee a little bit above the joint line. Frequently, the person with ITB pain has increased the amount they run (especially downhill), or they have changed something about their training (footwear or route).
For the longest time, injury to the ITB was called iliotibial band friction syndrome. The idea was that an excessively tight ITB would cause friction over the bone on the outside of the knee. More recent research suggests that friction isn’t really the issue, but pain in the ITB is more likely due to compression or impingement. Specifically, the ITB compresses a highly innervated fat pad between the band and the bone when the knee is flexed past thirty degrees. What is interesting about this is that the actual pain might be coming from the compression of the fat pad and not necessarily the ITB itself.
 Treating ITB Pain
Treating ITB Pain
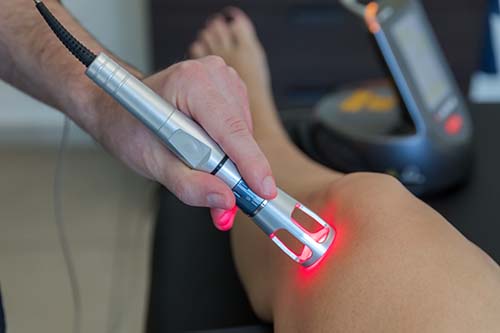
Although some patients with ITB pain might display weakness in the gluteal muscles, we cannot conclude that ITB pain is caused by this weakness. What is more likely is that a person gets weakness in hip abduction because of the ITB pain. Despite the lack of a biomechanical explanation for hip strengthening, patients seem to improve with this approach, so it might be worth a try. Commonly used treatments for ITB pain include foam rolling, ITB stretching, hip strengthening and soft tissue release. Laser therapy might also reduce symptoms in the area. The research hasn’t really given us a definite way to treat this condition, so it’s often a trial-and-error situation using a combination of practitioner experience and patient preference. Progressive overload and graded exposure seem to be a reasonable approach to many conditions, and ITB pain is one of them. Perhaps what has changed over the years are the recommendations for treatments that compress the area. For example, foam rolling has been used for many years, but since newer research has shown ITB pain to be an injury that stems from over-compression of the area, added compression with a foam roller doesn’t make much sense. Other options for changing the course of this condition include altering running biomechanics (trying a wider step width) and running with a higher cadence.
Summary
In short, pain in the iliotibial band is a common running injury and is not normally a difficult condition to diagnose. Recovery usually requires a discussion regarding loading the tissue (running volume), some strengthening, some clinical treatment and the avoidance of compression, such as with foam rolling. If you have ITB pain, we can help!
References
Hutchinson L, Lichtwark G, Willy R & Kelly LA. The Iliotibial Band: A Complex Structure with Versatile Functions. Sports Medicine 2022; 52(5): 995-1008
Ellis R, Hing W, Reid D. Iliotibial band friction syndrome—a systematic review. Man Ther 2007; 12: 200–8.
Fairclough J, Hayashi K, Toumi H, et al. Is iliotibial band syndrome really a friction syndrome? J Sci Med Sport 2007; 10: 74–6.
Geisler PR, Lazenby T. Iliotibial band impingement syndrome: an evidence-informed clinical paradigm change. Int J Athl Ther Train 2017; 22: 1–11.


 Treating ITB Pain
Treating ITB Pain