My Recent Experience with Lower Back Pain
By: Dr. Kevin McIntyre B.Kin., DC
It’s fair to say that chiropractors are experts in lower back pain. Much of the four-year program is geared toward the diagnosis and management of lower back pain. The one thing the curriculum cannot teach though is exactly what lower back pain feels like. Unfortunately, but also, fortunately, I recently experienced a short episode of lower back pain. I can now relate to some of the things my patients describe to me daily. It’s important to acknowledge that every case of lower back pain case is different. The following is just a synopsis of my recent experience which may have similarities with common presentations of uncomplicated mechanical lower back pain.
The Cause
I do not have a history of lower back pain or spinal injury. I did not injure my lower back by doing anything spectacular. I was sitting on a stool for about an hour. In hindsight, I realize that I was probably twisting my spine while I was sitting for too long. What I experienced was a very sudden sensation of tightening in my upper gluteal muscles. I stood up from the stool and then felt an immediate tightening in the lower back. It felt like a painful stretch when I bent forward, and there was little to no pain extending backward. I did not experience any other symptoms in the hips, legs or lower back.
The Diagnosis
It’s important to recognize that I didn’t have a mechanism that could reasonably damage any spinal tissue. I didn’t tear any muscles, tendons or ligaments. I didn’t sprain any joint structures or have any cause for fracture or “damage” to my lower back. Given this, I would say I “irritated” my lower back. Realistically, at 45 years old, I likely have some mild, age-appropriate degenerative changes. I must admit that I don’t often do rotational strengthening in the muscles of my lower back, and I don’t often sit for so long at a time. Taking these factors into consideration, it’s reasonable that my lower back got sore. It was irritated, sensitized and painful, but not damaged and nothing was broken.
The Management
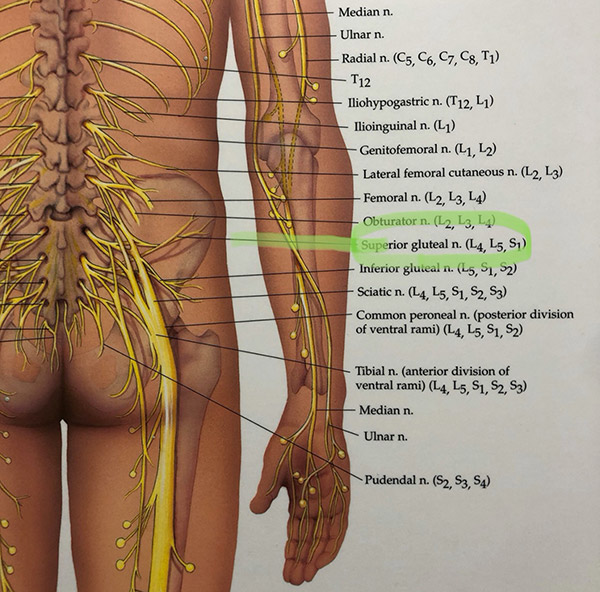
I’m writing this blog about four days after the onset of symptoms, and I would say I’m 90% better. I’ve returned to riding my stationary bike and careful weight training. I’m being careful with my movements and I’m doing gentle range of motion exercises. I’m being mindful of things I lift and really limiting my end-range rotational movements and lifting with rotation. For treatment, I did two sessions of active release and some laser therapy to my lower back. Perhaps what was most important for my quick recovery were the things I did not do. I didn’t stretch or continue with vigorous exercise. Although my pain felt muscular, I knew this is common and there wasn’t a mechanism to really damage my muscles. I believe the prolonged sitting and rotating irritated the discs in my lumbar spine and put the nerves in the area on “high alert”. I believe that most of my pain in the upper gluteal muscles was likely attributed to irritation of the superior gluteal nerve. (See the picture below).
X-rays were not necessary. Statistically, I likely have mild degenerative arthritis in the lower levels of my lumbar spine. This might make it reasonable to expect occasional irritation of these areas (more than when I was in my twenties), and sitting with rotation is a reasonable mechanism to cause it. It’s less reasonable to think I strained my gluteals from sitting.
I believe the irritation of the superior gluteal nerve (from L4-5, L5-S1) caused my muscular symptoms. This is important to consider. Many patients come to our clinic describing pain in this area and insist that their pain is muscular. At the same time, their symptoms have become chronic, and they are constantly stretching the gluteals to relieve the feeling of tightness and pain. If my theory is correct, stretching my gluteals in my situation might continue to irritate my lower back and perpetuate the nerve sensitization. In this instance, stretching is unlikely to help too much and might even prolong the irritation. In my case and many cases of uncomplicated lower back pain, a better strategy is to keep moving but don’t irritate the area. This is where a knowledgeable professional is helpful. They can help you figure out the activities and movements that might be helping or aggravating your lower back pain. These instructions are different for everyone, and every diagnosis has a different set of recommendations.
The Prognosis and Prevention
My lower back pain recovered very quickly. This tells me there was likely no tissue damage but again, just an irritation of the area. I don’t have a history of lower back pain, so I don’t expect it to occur again. It’s true, my spine will degenerate as I go through life, but that certainly doesn’t mean I will have lower back pain again. For prevention, it would be wise for me to teach my lower back to tolerate rotational movements and to strengthen the muscles responsible for this movement. I can build capacity for that movement in a safe, controlled manner to build up my spine rather than keep it susceptible in this movement direction. At the end of the day, sitting for prolonged periods and rotating mindlessly is a good way to aggravate any lower back. Many cases of lower back pain do not have to last very long or be a major inconvenience if the proper steps are taken. Pain does not equal damage!
Are you experiencing lower back pain? We can help! Give our clinic a call at 905-220-7858 or email us at info@burlingtonsportstherapy.com