Osteoarthritis and Rheumatoid Arthritis – What’s the Difference?
There are many different types of arthritis. One thing they all have in common is that there is a joint (“arth”) that is inflamed (“it is”). For this week’s blog we’re going to differentiate between the two major classifications of arthritis; osteoarthritis and rheumatoid arthritis.
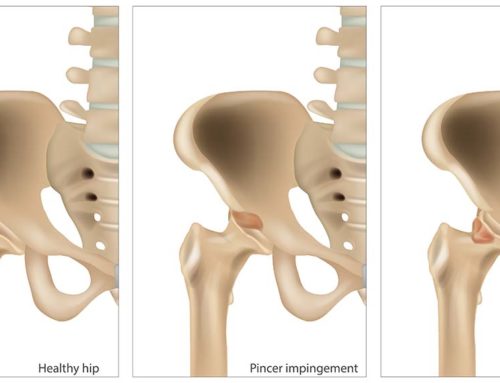
Osteoarthritis
The most common form of arthritis is degenerative arthritis, also called osteoarthritis. As the name implies, the joint surface has some “wear and tear” in it. In fact, most people over the age of 40 likely have some elements of joint wear and tear, so they actually have “arthritis”. The word doesn’t have to be so scary. Many people are still able to remain very active, despite having significant degeneration in a joint. Degenerative joint disease is characterised by a non-inflammatory wearing of the joint cartilage. It can be painful, causing the feeling of stiffness and it can swell. Usually lab tests are negative (bloodwork) and the person notices stiffness in the area after prolonged positions. For example, when you stand up after a long flight and your knees are stiff, achy…this could be arthritis! Osteoarthritis is very common in the lower neck and the lower part of the lower back. The knee is also very common, especially the inside area of the joint. Genetics play a role, as does the activities that you do. Your sport, your job, previous trauma…these all factor in to how a joint can become degenerated.
Rheumatoid Arthritis
Rheumatoid arthritis is different from degenerative arthritis. Although there is a genetic link, your sport, your job, previous trauma; these don’t really factor in as much. Rheumatoid arthritis is more of a systemic condition that affects various tissues related to joints. Essentially, someone with rheumatoid arthritis has an immune system that chooses to attack its own joints. Because of this, it doesn’t really pick a “right knee” or a “left ankle”. It chooses characteristic joints that it likes. For example, in the hands it likes to target the proximal interphalangeal joints (middle knuckle) but spare the distal interphalangeal joints (the last knuckle in the finger). So when we have someone that has swelling and pain in multiple fingers, in both hands including the middle knuckle but not in the last joint of the finger, it’s unlikely that this is strictly from wear and tear. It is highly suspicious that the person’s immune system is attacking the joints and has targeted the middle joints of the fingers. Other symptoms of rheumatoid arthritis include pain, redness and swelling in symmetric joints (left and right of the same joint) occurring simultaneously. Morning stiffness, pain with movement, tenderness and tender nodules in the soft tissues are also symptoms of rheumatoid arthritis.
Usually rheumatoid arthritis (RA) begins between 20-60 years of age. Pain and symptoms are most common in those over 40 to 50 years of age. The symptoms can come and go but for some, they persist constantly. Some blood tests can be indicative and some changes on x-rays are also helpful in distinguishing rheumatoid arthritis from osteoarthritis (degenerative arthritis). (A reminder for the practitioners out there; x-ray changes include marginal erosions and a uniform loss of joint space).
Treatment for arthritis varies. The type of arthritis and the severity of the changes are perhaps the most important variables for treatment. Regardless, Burlington Sports Therapy treats many different types of arthritis on a daily basis. We can help. Give us a call at 905-220-7858 so your arthritis can be diagnosed properly and your treatment options can be discussed with you.