Sciatic Pain and Dermatomes
There are many different causes and types of back pain and there are many different structures in the spine that can become irritated and generate pain.
Radiculopathy (Sciatica)
One important distinction that might impact the course of recovery is whether there are any leg symptoms of a neurological nature. The medical term we use to describe these symptoms is radiculopathy, but the more commonly-known term is “sciatica”. Radiculopathy is normally characterized by symptoms of numbness, tingling, pins and needles, weakness and pain (dull or sharp). As you can see, the symptoms can be quite variable! Lower back pain without any signs or symptoms of radiculopathy typically has a more favourable course. Lower back pain with an associated radiculopathy usually has a poorer prognosis. For many people, the symptoms of radiculopathy are more uncomfortable than the lower back pain that is occurring.
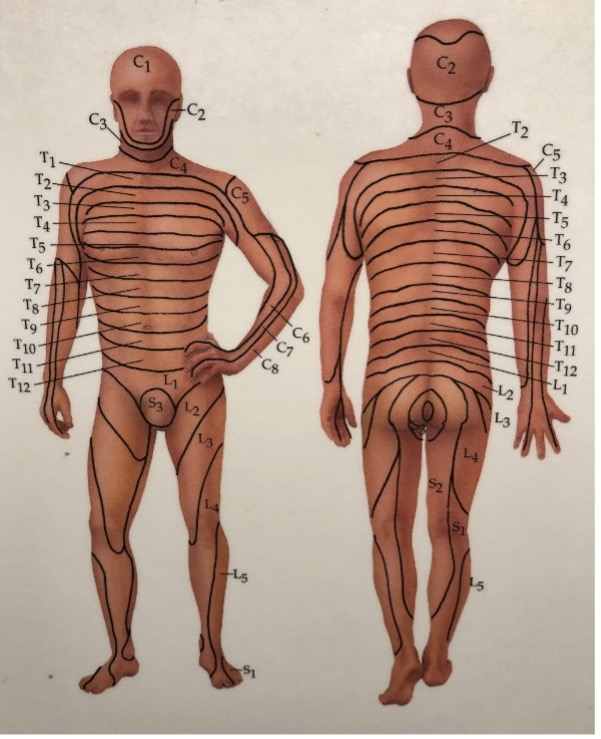
Dermatomes and Dermatome Maps
When a patient presents with symptoms that extend from the lower back and down the leg, many practitioners become curious as to where in the leg or foot the symptoms are occurring. This can give clues as to what nerve is involved and then we can determine what level of the spine may be at fault. Perhaps then the treatment can be more specific to the area of the spine that is causing the problem.
A dermatome is a medical term that we use for localizing these symptoms. A dermatome refers to the area of the skin that the person is experiencing symptoms in a pattern that has been established as characteristic for a certain spinal level. For decades medical and rehabilitation textbooks have dermatome diagrams that can help practitioners figure out what level of the spine is involved when a patient points to a certain distribution of symptoms. Can these dermatome charts be trusted though?
An interesting 2019 study looked at 93 patients with radiculopathy. These patients had nerve root irritation affecting the L5 and/or S1 nerve roots (which is very common). 18 practitioners (6 physio, 6 MD and 6 chiropractors) examined the dermatome patterns in these patients and in the end, they were only correct 50% of the time!
Dermatomes can be used as an approximate at best. Perhaps best to use it as a general idea for whether a patient has nerve root irritation or not. It would not be supported by the evidence to use clinical symptom patterns in order to determine which spinal level is involved. We can use dermatomes to help assist us in knowing whether a person has radiculopathy, but we can’t confidently tell a patient at what specific level of their spine may be the cause since there is a lot of variability. The good news is that under most circumstances it shouldn’t impact a practitioner’s ability to provide evidence-based care and assist the patient in overcoming their pain.
Evidence-informed Practice
At Burlington Sports Therapy we pride ourselves on being evidence-informed practitioners. Through an effort to keep abreast of the best available literature, we strive to provide better treatment and give better recommendations to our patients. Perhaps contrary to what we were taught in school, newer research has shed light on the reliability of the traditional dermatome charts. They are not useless, but perhaps we can say that there’s a lot of overlap in dermatomes. Dermatomes vary considerably among different people and radicular pain may not follow these dermatomal patterns.
If you’re experiencing lower back pain, please give us a call, we can help!
By Dr. Kevin McIntyre B.Kin., DC
References
Albert HB, Hansen JK, Sogaard H & Kent P. Where do patients with MRI-confirmed single-level radiculopathy experience pain, and what is the clinical interpretability of these pain patterns? A cross-sectional diagnostic accuracy study. Chiropractic & Manual Therapies 2019; 27: 50.
Murphy DR, Hurwitz EL, Gerrard JK, Clary R. Pain patterns and descriptions in patients with radicular pain: does the pain necessarily follow a specific dermatome? Chiro Osteopath 2009; 17:9.
Taylor CS, Coxon AJ, Watson PC, Greenough CG. Do L5 and S1 nerve root compressions produce radicular pain in a dermatomal pattern? Spine 2013; 38(12): 995–8.